 In the UK, all pregnant women are provided with support from their local midwifery team throughout their pregnancy. This involves a series of appointments, tests, and scans that start from when you are about 8 weeks pregnant and continue until after your baby is born. Whilst many NHS trusts will try and offer you appointments with the same midwife throughout your pregnancy, you may find that you see a number of different professionals.
In the UK, all pregnant women are provided with support from their local midwifery team throughout their pregnancy. This involves a series of appointments, tests, and scans that start from when you are about 8 weeks pregnant and continue until after your baby is born. Whilst many NHS trusts will try and offer you appointments with the same midwife throughout your pregnancy, you may find that you see a number of different professionals.
Taking Time Off Work For Antenatal Appointments
UK mothers-to-be are legally entitled to paid time off for antenatal care. This includes appointments with your midwife, scans, antenatal and parenting classes if these have been recommended by a GP or midwife, as well as any other medical appointments that may arise as a result of your pregnancy.
Registering With The Community Midwives
Once you have got a positive pregnancy test you will need to be registered with your community midwife team. These midwives will support you during your pregnancy and for a few days after your labour. In many areas you can refer yourself directly to the team but if you are not sure you can check with your GP surgery.
First Appointment – The Booking Appointment (8-9 Weeks)
In some areas, you may need to have an initial appointment with a GP or midwife to confirm your pregnancy, however, for most women, the first appointment with a midwife will be what is known as the “Booking Appointment”. This will usually take place when you are around 8 to 9 weeks pregnant and takes approximately one and a half hours. You may be provided with your green maternity notes (a green booklet with all of your personal information relating to you and your pregnancy) prior to this appointment and will be asked to fill in certain sections to bring with you. It is important that you bring these notes with you to every appointment and eventually to the place where you give birth. Most women carry the notes with them everywhere during the last trimester, just in case.
You will be asked about your own, your partner’s and your family’s medical history, as well as lifestyle information such as whether or not your smoke, any exercise or drinking habits. It’s important that you answer all of the questions honestly as this will help your midwife to determine if your pregnancy should be considered to be of a higher risk of complications. You will also be weighed and asked your height and your Body Mass Index will be calculated.
You will also be given information about the screening tests that are available for your pregnancy, such as that for Downs Syndrome, and you will be asked to provide a blood sample to test for various diseases and conditions. In addition, you will be given information about ante-natal classes, and the options that are available to you regarding where to give birth, although you don’t need to make any decisions at this point.
Testing For Medical Conditions
During your first appointment you will be asked to consent to a number of tests. Whilst you are within your rights to decline any of these tests, they do allow you to be fully informed about the health of both yourself and your baby, and any risks that may be involved in your pregnancy to you and your baby.
Blood Pressure
Your midwife will measure your blood pressure at your first and every subsequent appointment. A wrap is placed around your arm and inflated. Sometimes a machine’s sensor is used to measure your blood pressure, whilst in other cases the midwife will use a stethoscope and listen to changes in your heart rate to determine a reading.
A blood pressure reading consists of two numbers, for example 120 / 80. The first number is your systolic blood pressure, which is when the heart is beating and moving blood around your body. The second number is your diastolic blood pressure, which is the pressure of your blood in between your heartbeats. Most healthy people tend to have a blood pressure reading of between 110/70 and 120/80.
In the early stages of your pregnancy, your blood pressure is likely to decrease as a result of hormone changes. This is what causes the feelings of dizziness and fainting that many pregnant women experience during the first trimester. During the second trimester, it is likely that your blood pressure will start to increase again.
If your blood pressure is high (i.e. 140/90 and above) your midwife will likely want to carry out more tests, perhaps by monitoring your blood pressure every few hours. This is because high blood pressure (also known as hypertension) can be a sign of pre-eclampsia, which is a condition that results in a reduced flow of blood to the placenta, reducing your baby’s supply of oxygen and nutrients. Therefore, it is important to have your blood pressure taken during every appointment with your midwife.
Urine Tests
You will also be asked to provide a urine sample at your booking appointment and every subsequent appointment with your midwife. This will be tested by the midwife for the presence of protein, white cells, and glucose (sugars) by using a dip-stick that changes colour if something is detected. If protein or white cells are detected in your urine it could indicate the presence of a bacterial infection which can be dangerous for you and your baby during pregnancy, or it could indicate pre-eclampsia. If glucose is detected this could indicate the development of gestational diabetes, which is a condition that results in your blood sugar levels being too high and can cause complications during pregnancy and labour. If necessary, your urine will be sent for further testing and you may need to start some sort of treatment. Your midwife will probably supply you with a new sample bottle at the end of each appointment for you to bring to the next appointment.
Blood Tests
In your booking appointment your midwife will ask to take a sample of your blood to test for various conditions. Your blood will be tested for:
- Your blood group – If your blood group is Rhesus Negative and your baby has inherited the Rhesus Positive gene from his or her father there is a possibility that your body will start to produce antibodies in response to your baby’s blood cells. This is potentially dangerous and you will be offered treatment for this.
- Your immunity to Rubella (German Measles) – If you contract this disease in pregnancy it could damage your baby. If required, you will be offered a vaccination.
- Hepatitis B – If you are a carrier then your baby will be offered a vaccination once they are born.
- Syphilis – If required you will be offered antibiotics to treat this.
- HIV – If you are infected with HIV then the chances of you passing on your infection to your baby can be significantly reduced with treatment during your pregnancy.
- Thalassaemia – A disorder that affects your blood’s ability to carry oxygen which can be passed to your baby.
Depending on your medical history and circumstances you may be offered additional tests for other conditions including Sickle Sell, MRSA, and Chlamydia.
First Scan – The Dating Scan (12 Weeks)
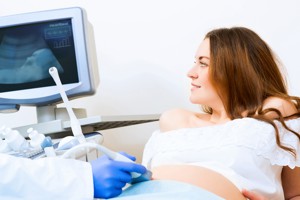 In the UK, pregnant women are offered two ultrasound scans as standard. This first of these will be when you are around 12 weeks pregnant and is known as the Dating Scan. You may be offered additional scans if there are any concerns about you or your baby that require further investigation. You do not have to have any scans if you do not want to.
In the UK, pregnant women are offered two ultrasound scans as standard. This first of these will be when you are around 12 weeks pregnant and is known as the Dating Scan. You may be offered additional scans if there are any concerns about you or your baby that require further investigation. You do not have to have any scans if you do not want to.
During the Dating Scan and any subsequent scans a specially trained sonographer will use an ultrasound device to create an image of your baby in the womb. A probe with ultrasound gel is placed on your stomach and this generates images that appear on a screen. The room will probably be dimmed in order to allow the sonographer a better view of the images that are created. There are no known risks to the mother or baby from an ultrasound scan.
You will probably be asked to drink a good amount of fluids one hour before your appointment and you will need to avoid passing urine in order to ensure that your bladder is full during the scan. This is because at this early stage of pregnancy your baby is cradled very low in your pelvis and difficult to see with ultrasound. Having a full bladder lifts up your uterus into a more viewable position.
During your 12 week scan, the sonographer will take measurements of the baby in order to determine your due date. Whilst you might have an idea of your due date based on the date of your last period, the scan is generally considered more accurate and the date that is determined here will be used for all future appointments and medical decisions about your baby. The scan will take about 15 – 20 minutes. A growth chart will be produced based on the measurements taken at this scan. This will then be used by your midwife to plot and monitor your baby’s growth.
You will also be offered a screen for Downs Syndrome during this scan. You do not have to have it if you do not wish to do so. Measurements will be taken and based on that a risk score of the baby having Downs Syndrome will be calculated. If the score is high enough then additional, more accurate tests may be offered.
Can Someone Accompany Me To The Scan?
Yes, in fact, it is a good idea to have your partner or close family member or friend with you during the scan as it may be distressing for you if any problems are detected. If you have additional children, most hospitals will not allow them to attend with you, but check in advance if you are not sure.
Will I Get A Picture?
Most hospitals will provide you with one or more pictures of your baby, however, many do now charge for this service.
The 20 Week / Anatomy Scan
The second standard scan offered to mothers-to-be in the UK usually takes place when you are 20 weeks pregnant. This is known as the anatomy scan and the sonographer will check various parts of your baby’s body for any abnormalities or conditions. This scan will take about 30 minutes, depending on the position of your baby. Sometimes, the sonographer may not be able to check all of the parts of your baby’s body as required because of the way your baby is lying in the womb. You may be asked to empty your bladder or jump around to try and encourage your baby to move. If it is still not possible to check all of the areas your sonographer will arrange for you to have an additional scan appointment. This does not necessarily mean that anything is wrong, it is just often difficult to get clear images of every part of your baby’s body.
During this scan you will be asked if you wish to know the gender of your baby. It is entirely up to you whether or not you wish to know this information. However, if you do decide to find out, your sonographer may not necessarily be able to identify your baby’s gender due to their position in the womb.
If the sonographer detects any problems with your baby during the scan, such as an issue with his or her spine or heart, then you will probably be offered further tests.
Additional Appointments
As your pregnancy progresses, you will have regular appointments with your midwife. Unless you have additional medical concerns, your appointments will probably take place at the following stages:
- 16 weeks
- 24 weeks
- 28 weeks
- 31 weeks
- 34 weeks
- 36 weeks
- 38 weeks
- 40 weeks (and 41 weeks if you have not already given birth)
If this is your second baby, then you may not be offered an appointment at 24 weeks, 31 weeks, and 40 weeks, however, your midwife may ask you to attend these appointments if she has any concerns, or if your particular NHS trust has a different policy.
At each of these appointments your midwife will test your urine and your blood pressure, discuss any concerns that you might have and give you the results from any scans or tests if required. From 24 weeks you midwife may use a Doppler device to allow you to hear your baby’s heartbeat. Many midwives will allow you to make a recording of this using a smartphone. From 28 weeks your midwife will measure your bump to see how the baby is growing based on the information provided by your scans. If you are measuring small or large then you may be sent for an additional scan.
Your blood will be tested again for infection and iron levels at 28 weeks. Low iron levels could indicate that you are anaemic, which can cause problems during labour such as excessive bleeding. If needed, you will be prescribed additional iron supplements.
Testing For Gestational Diabetes (24 / 28 Weeks)
Gestational diabetes is a condition that affects your blood sugar levels and can result in a larger baby that requires you to have a caesarean section, as well as other complications. The condition tends to develop during the second trimester, which is why testing is carried out at either 24 or 28 weeks.
You may be offered an Oral Glucose Tolerance Test (OGTT) for gestational diabetes if you have been assessed as being of higher risk of developing the condition or glucose has been detected in your urine. Your risk of developing gestational diabetes is higher if you fall into any of these categories:
- You have experienced gestational diabetes in a previous pregnancy
- You have previously given birth to a baby who was over 4.5kg (10lbs) in weight
- Your Body Mass Index (BMI) is 30 or higher
- You have parents or siblings with diabetes
- You are of South Asian, Black Caribbean, or Middle Eastern ethnic origin
The OGTT involves a period of fasting, followed by a blood test, followed by the consumption of a glucose drink, followed by an additional blood test. Many women can control gestational diabetes through diet alone, however, in some cases regular insulin injections are required.
Preparing For Labour – 34 Weeks Onwards
From 34 weeks onwards, your midwife will start discussing your birth plan with you, and post-labour issues such as breast-feeding and keeping healthy after birth. If you require an appointment at 41 weeks then the options for induction of labour will be discussed with you. You can choose to refuse labour inductions methods but if your pregnancy continues beyond 42 weeks then you will be monitored every two to three days.
Post Labour Visits
 You will remain in the care of your Community Midwife Team for several days after you have given birth. Your midwife will visit you at home, usually the day after you have come home with your baby, and then may visit every two to three days depending on your and your baby’s needs until around day 10. This varies from NHS trust to trust.
You will remain in the care of your Community Midwife Team for several days after you have given birth. Your midwife will visit you at home, usually the day after you have come home with your baby, and then may visit every two to three days depending on your and your baby’s needs until around day 10. This varies from NHS trust to trust.
Your midwife will check your baby’s weight and health to ensure that he or she is developing well. She will also check your own health, for example, if you required stitching following labour she may check how this is healing, or she may ask you about your mental health if you are feeling particularly low or upset. Your midwife can offer you advice and support about breast-feeding if you require it.
After which, your child will be passed onto the Health Visiting Team who will provide support to your child until they reach the age of 5. Your health visitor will offer your child regular checks for their weight, and as well as regular development checks. They can provide support for any queries you may have concerning your child’s health and growth.
